Thinking outside the brain to advance CNS drug development
CNS diseases can have a wide range of symptoms which can make them difficult to diagnose and treat based on clinical presentation alone. Biomarkers can provide objective measures of the underlying disease process, which can help to distinguish between different subtypes of the disorder so that targeted therapies can be aligned with the right patients. They can also be used to predict and monitor treatment response across heterogeneous patient populations – in which disease response and the way patients process the drug can vary greatly – and to determine when to adjust or discontinue therapy.
Traditionally the CNS field has relied heavily on the use of neuroimaging biomarkers such as amyloid beta, as used in the trial of the recently approved lecanemab for the treatment of Alzheimer’s disease. The challenge is that these biomarkers can have limited sensitivity and may not be able to detect subtle changes in brain pathology or function that associate with early disease progression or treatment response. The expense of these scans also limits longitudinal sampling and the ability to assess changes in patients over long treatment durations of months or years, barring a costly population-level approach. For example, CT and MRI do not measure amyloid and so scans must be done with PET imaging, which is not available for routine care.
Genetic biomarkers can be used to identify specific gene mutations or variations associated with a particular disorder, but these are largely static measures that can again be limited in their ability to predict the course of the disease or response to treatment over time.
New biomarkers that can read out the real-time dynamics of the brain, and how those dynamics are modified with therapy, are needed – particularly those that enable detection of changes earlier in the disease process and/or treatment period so interventions can be optimized. For these reasons, small molecule biomarker discovery in the CNS field has become increasingly prevalent in recent years.
The blood: a rich resource to capture new CNS biomarkers
In the context of CNS drug development, small molecule biomarkers are typically used to measure the levels of specific metabolites in the brain, such as neurotransmitters, amino acids, and lipids, to assess biochemical changes that occur in the brain in response to a particular disease or treatment. Because they reflect both host biology and underlying disease biology, small molecules have the potential to provide unprecedented views into the factors that modulate CNS disease onset and progression. They can be dynamic, sensitive indicators of disease specific processes and drug response.
Still, the use of small molecule biomarkers in CNS drug development has been limited to date. A key reason is that traditional methods of capturing and analyzing metabolites in the brain are highly invasive. They can be obtained from cerebrospinal fluid (CSF) via lumbar puncture, or via biopsy of the brain or other CNS tissue, but these approaches cause significant risk and discomfort to patients and are typically reserved only for those with severe or advanced stages of the disease.
Luckily, evolving research has opened the door wider for another, non-invasive route of capturing metabolites that originate from the CNS: the bloodstream.
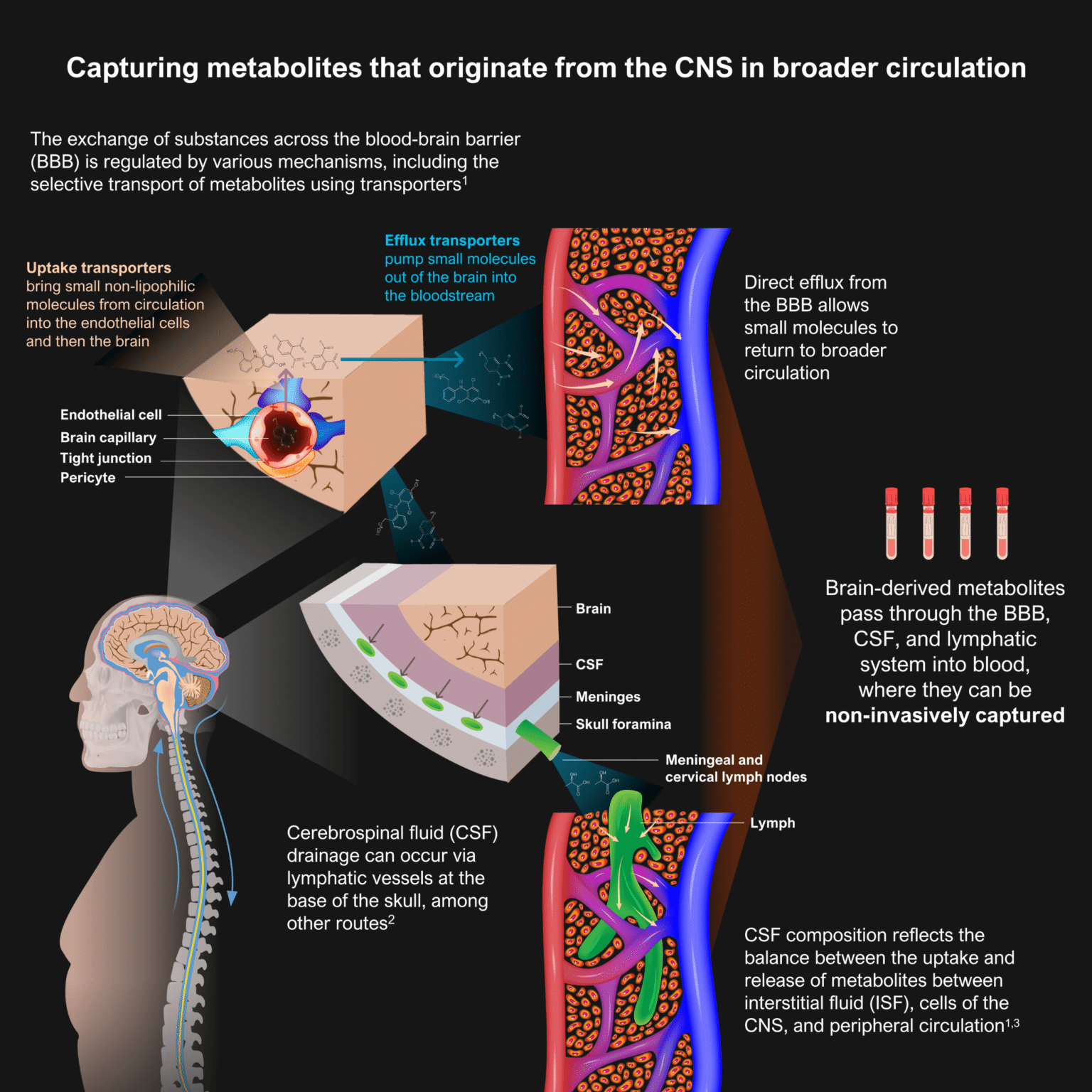
The blood-brain barrier (BBB) is a selectively permeable barrier that regulates the exchange of molecules between the blood and the brain. Historically it was thought that only a limited number of small lipophilic molecules could cross from the brain into broader circulation, largely limiting the discoverability of CNS metabolite biomarkers to brain tissue or CSF. However, a large body of work has now demonstrated that there are transporters that enable the selective exchange of nutrients, ions, peptides, drugs, and hormones directly between the brain and blood. Uptake transporters can bring small non-lipophilic molecules from the peripheral circulation into endothelial cells and in turn, the brain, while efflux transporters can pump small molecules directly out of the brain to the blood.
Because CSF is in direct contact with brain tissue, this fluid can also reveal metabolic changes happening in the brain. Its composition reflects the balance in uptake and release of metabolites between the cells of the CNS and peripheral circulation. Newer studies suggest that meningeal lymphatic vessels absorb CSF from the adjacent subarachnoid space and brain interstitial fluid (ISF) via the glymphatic system, thus acting as a drainage route for CSF into blood.
This growing body of research is important because it expands the scope of potential brain-derived biomarkers that can be captured in blood to monitor brain metabolism, inflammation, and other biological processes in CNS diseases.
Finding new biomarkers for CNS diseases: don’t get stuck in the head
It is clear that non-invasive profiling of metabolite biomarkers can bring many new advantages to CNS drug development programs, including:
- Early detection: Circulating biomarkers can be used to detect changes in the brain at earlier stages of disease processes, including in at-risk populations or during prodromal stages prior to the manifestation of clinical symptoms or syndrome. This can aid in early diagnosis as well as optimization of prevention and intervention strategies to improve outcomes.
- Treatment response monitoring: Small molecule biomarkers can be used to predict individuals who are most likely to respond to specific drugs, and can also be measured throughout the treatment period to dynamically optimize dosing and timing of a drug and/or to discontinue therapy in patients that have no response.
- Complementary insights: Metabolite biomarkers can be used in combination with other biomarkers such as neuroimaging or genetic biomarkers to provide a more comprehensive understanding of the CNS disease and treatment response
With high-throughput technologies now available to enable rapid, large-scale small molecule biomarker profiling in blood, the potential to discover new CNS biomarkers has grown exponentially. Sapient’s next-generation mass spectrometry-based platform can assay more than 11,000 small molecule biomarkers per biosample, performing nontargeted screening to identify metabolites of interest. We can then elucidate the specificity of key biomarkers through biocomputational analysis and by referencing our Human Biology Database to confirm them as originating from the brain. We also have the ability to perform structural elucidation of unknown molecules that have been identified, and a follow-on technology pipeline to develop targeted assays for priority molecules under regulated controls. This allows for faster translation of discoveries to accelerate biomarker-guided CNS drug development.
To learn more about how Sapient can support your CNS drug programs, request a meeting with our scientists.